Procedures of Aesthetic Vaginal Surgery
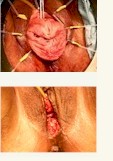
Vaginoplasty (vaginal rejuvenation)
This aesthetic vaginal surgery aims to tighten lax muscles and tissues and remove excess vaginal skin to narrow the diameter of the vagina resulting in a smaller and tighter opening and vaginal canal. The tightening is done in the entire length of the vagina and not merely the opening few centimeters. Dr. Alinsod does full depth repairs unlike the superficial perineoplasty repairs done by most plastic surgeons and gynecologists. This can be done in the surgery center under general or spinal anesthesia or under local anesthetic with some sedation. However, Dr. Alinsod has refined the in-office vaginal rejuvenation surgery that does not require an IV and is done under mild sedation and local anesthesia. He use the Ellman Surgitron Radiofrequency device to make exceptionally precise and minimally traumatic incisions. This method is dramatically less destructive than the use of Yag lasers. It takes about 60 minutes to perform. Many advertise this procedure for the “Enhancement of Sexual Gratification” as well as a cosmetic procedure.
Perineoplasty (Perineorrhaphy)
The visible area between the vagina and the rectum is called the perineum. This is the region where episiotomies are cut and where tears during childbirth are most common. Perineoplasty (or Perineorrhaphy) aims to make this region appear normal by excising excess skin, loose skin tags, and suturing the underlying muscles or the perineal body closer together to give a more snug feeling in the introitus or vaginal opening. Most plastic surgeons who perform vaginoplasty surgery are actually performing perineoplasty surgery, a more superficial procedure that does not tighten the entire depth of the vaginal canal. This procedure has been advertised by many to “Enhance Sexual Gratification.” The procedure almost always accompanies vaginoplasty since you are working in the same area. This procedure takes 30 minutes to perform.
Labiaplasty Minora (Labial Reduction)
This surgery is for the removal of excess, floppy, or uneven labia minora (smaller interior vaginal lips) that often causes chronic irritation, rubbing, or discomfort during sexual intercourse. Many request this surgery to eliminate the appearance of a bulge with certain clothing such as wet swimsuits or leotards. The term “Labiaplasty” can also relate to the cosmetic surgery of the labia majora (larger outer lips) to make it less prominent and saggy. Labias can grow large with estrogen stimulation at puberty and pregnancy and with the effects of gravity with aging. Labiaplasty is done in the operating room and in the office under local anesthesia at dramatically decreased costs. The Ellman Surgitron is also the tool of choice. It is dramatically less destructive than lasers often advertised. This procedure takes 60 minutes to perform.
Labiaplasty Majora
The broader outer lips of the vulva can be enlarged with excess skin and tissue. This enlargement can cause an embarrassing bulge in pants, swimsuits, or leotard. It can also increase the discomfort of sweating in the vulva. The labia majora may be enlarged from birth, secondary to childbirth, or due to aging. Many women also find quite a large and droopy labia majora after major weight loss such as post bariatric surgery. Dr. Alinsod has refined his technique over the years to safely reduce the size of the labia majora by exicing a crescent shaped portion of the inner portion of the labia majora. The scar is hidden in the crease between the inner and outer labia. Labiaplasty is done in the operating room and in the office under local anesthesia at dramatically decreased costs. This procedure takes 60 minutes to perform.
Clitoral Hood Reduction
Excess skin on the sides of the clitoris often causes the clitoris to look enlarged or uneven. Genetics, estrogen, and testosterone exposure can make significant changes in the way the clitoral area appears. A labiaplasty itself may result in the appearance of a relatively larger clitoral area since the excess labia have been removed drawing the eyes to the clitoral region. Dr. Alinsod offers an exceptionally precise surgery for women seeking to improve the aesthetic appearance of their genital area by excising the extra folds of skin lateral to the clitoris. The clitoris itself and its nerves are never touched. This is NOT clitoral mutilation or clitoral un-hooding. Clitoral Hood Reduction is done in the office under local anesthesia. The procedure takes 30 minutes to perform.
Hymenoplasty
This surgery is the reconstruction of the hymen. Cultural, religious, or social reasons predominate when this surgery is contemplated. Hymenoplastyis performed to make the patient appear virginal. It works for women who have not had vaginal deliveries, and preferably, in those who have never been pregnant. We take advantage of the Ellman Surgitron to make extremely precise incisions into the vagina and remnants of the hymeneal ring to bring them into close approximation to allow delicate sutures to hold the tissues in place. Once healed, the act of sexual intercourse can result in bleeding when the hymen is torn or stretched. Hymenoplasty is done in the office under local anesthesia. This procedure takes 60 minutes to perform.
Laser Resurfacing
CO2 lasers have been used for over 20 years to ablate lesions in the vaginal area. Examples include venereal warts and skin tags. They have also been used to treat precancerous vulvar, vaginal, and cervical lesions. We often marveled at the beautiful new tighter skin that grew after a laser treatment. We have used the CO2 lasers since 1986 with excellent success. Now, the CO2 laser is getting more acceptance by other gynecologists as a tool for cosmetic vaginal rejuvenation and resurfacing. Other lasers that have been used in the vaginal region include the Yag lasers of varying wavelengths. New lasers and light sources are also available. The new “Fractional” or Fraxel-type of lasers can regenerate collagen, smoothen skin, and reduce scarring without the downtime. We also have Deep IR (Infrared) heating used to tighten the skin and reduce sagging. Laser Resurfacing is done under local and topical anesthesia in the office. Laser resurfacing takes 15 to 30 minutes to perform.
Incontinence Sling
The urethra is the tube that drains the bladder. The urethra is where you see urine coming out. This structure may fall down just like the bladder does. This often results in leakage of urine when one coughs, laughs, jumps, or bends down. Repair of this organ often means you must place a mesh below it and support it to stop the leakage of urine. Many women have urethroceles with absolutely no symptoms. No surgery is needed in these asymptomatic patients. However, when symptoms occur, new minimally invasive technologies have been developed.
The newest and safest trend to deal with incontinence involves the use of polypropylene, an inert nylon-type material, that is placed right under the mid urethra to act as a backboard when one sneezes or coughs to then occlude or block the urethral opening and either decrease of stop the leakage of urine. These procedures are all called “Tension-Free” because the slings are not sutured into muscle, fascia, or bone and are just left alone for ones own fibroblast to ingrow and hold the mesh. You may hear the term TVT or TOT. They refer to the route the slings are placed. TVT, or tension-free vaginal tape can be placed through an incision right above your pubic bone. TOT, or transobturator tape, is placed through incisions on the crease of your inner thighs. These incisions are just about invisible. Both procedures are outpatient surgeries of about 15 to 30 minutes. Newer sling technologies have even eliminated the skin incisions and are placed totally vaginal using “short tape” technology. The success rates vary from 80 to 95 percent. Incontinence slings are done under general, regional, or local anesthesia in the surgery center or operating room. Most insurance companies cover this procedure. The cash cost of an incontinence sling is 4,000.
Cystocele Repair (Bladder Repair)
A cystocele is when the bladder falls down and often becomes visible. Urinary leakage often accompanies a cystocele. Cystoceles may cause pelvic pressure or just be unsightly. Cystocele repair (also called Anterior Repair or Anterior Colporrhaphy is the surgical reduction of the bulge to place the bladder back into its normal anatomic location. The traditional repair of plicating or overlapping tissues with suture unfortunately has a very high failure rate ranging from 25 to 60 percent. It is certainly one of the most challenging surgeries gynecologists and urogynecologists perform. More modern surgery treats cystoceles as a hernia of the bladder into the vagina, hence, the use of mesh or donor tissues as a patch or graft has been gaining steady acceptance. We have some of the most extensive experience in this type of surgery in the United States with success rates of about 90% in our hands. Cystocele Repair is done in the surgery center or operating room under general, regional, or local anesthesia. The procedure takes 60 minutes to perform. Most insurance companies cover this procedure.
Rectocele/Enterocele Repair (Rectal Repair)
When the bulge into the vagina comes from the rectum it is called a rectocele or rectal prolapse. As with other forms of pelvic organ prolapse (cystoceles, enteroceles, vaginal prolapse) childbirth, chronic cough, chronic constipation, and obesity are predisposing factors. Symptoms are similar to cystoceles such as pelvic pressure, an unsightly bulge in the vagina, and constipation. Furthermore, the need of reaching into the vagina to push stool out is not uncommon. A bulge into the vagina can also be caused by small bowel pushing the vaginal tissues. This is called an enterocele. It can occur at the same time as a cystocele and a rectocele. In fact, we often cannot tell what is causing the bulge in the vagina whether it is bladder, rectum, or bowel, or all! Modern repair uses mesh or donor tissue with excellent success found. This repair is technically quite challenging and few are trained in the modern repair of this problem. Surgical repair consists of using sutures to bunch up the bulging tissues together. More modern repair consists of the use of mesh or donor tissues. This newer method gives success rates of over 95% in our hands. Rectocele Repair is done in the surgery center or operating room under general, regional, or local anesthesia. The procedure takes 60 minutes to perform. Most insurance companies cover this procedure.
Vaginal Vault Suspension
A vagina that looses its support may come down and out into the open air. The degree of vaginal prolapse may vary from just having the top fall down a few centimeters to ones that completely go inside out. If a woman still has her uterus then this is called a uterovaginal prolapse. If only the uterus falls out and the top of the vagina is still well suspended then it is called a uterine prolapse. Vaginal vault suspension can be done in many ways. Some physicians prefer an abdominal approach to attach the top of the fallen vagina to the sacrum. Some highly skilled surgeons do this laparoscopicaly. The procedure is called a sacralcolpopexy. More often a vaginal approach is performed. The top of the vagina can be sutured to the uterosacral ligaments or to the sacrospinous ligaments. Either approach works well with different complications to consider. A newer procedure called the Posterior IVS (Intravaginal Slingplasty) has been developed in Australia and New Zealand, popularized in Europe, and now approved in the United States. This vaginal approach uses a polypropylene mesh that is attached to the top of the vagina and suspended “tension-free” via two small incisions near the anus and one incision in the vagina. You can view this procedure in my Video Library. The success rates of all methods are approximately the same at 80 – 90%. Vaginal Vault Suspension is done under general, regional, or local anesthesia in the surgery centeror operating room. Vaginal Vault Suspension takes 60 minutes to perform. Most insurance companies cover this procedure.
Uterine Suspension
When a firm mass is felt or a hard bulge is seen protruding out the vagina it usually a cervix and uterus prolapsing past the vaginal opening. This problem typically was treated with a hysterectomy or an abdominal procedure to shorten stretched out ligaments thereby “suspending the uterus and cervix. Dr. Alinsod has pioneered vaginal surgery techniques for uterine prolapse that is entirely vaginal in approach with no skin incisions. This technique has been taught world-wide. Uterine Suspension is done under general, regional, or local anesthesia in the surgery center or operating room. Uterine Suspension takes 60 minutes to perform. Most insurance companies cover this procedure.