PIGMENTED LESIONS
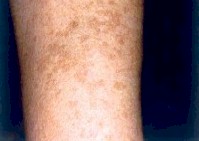 Before |
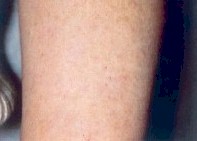 After |
The most commonly treated conditions of pigmented lesions are solar lentigines, also known as “age spots,” “liver spots” or “sun spots”; “café au lait birthmarks”; and freckles. These benign pigmented lesions are due to an excess of pigment in the skin, usually due to sunlight exposure and congenital factors.
The mechanism of pigmented lesion removal is based upon selective destruction of melanocytes and melanosome-containing epidermal keratinocytes. The lesion darkens and crusts after treatment, and is naturally sloughed off the skin within two weeks.
Age Spots/Sun Spots & Freckles
Freckles (also known as ephelides) are small flat brown spots that appear on sun-exposed skin, especially the face and arms. Freckles are inherited and become darker with consistent sun exposure. Ultraviolet rays from the sun activate pigment producing skin cells (melanocytes) to produce pigment (melanin). Increased melanin is manifested as dark or brown spots on the skin.
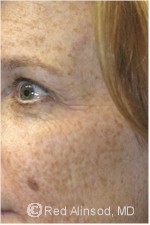 Before |
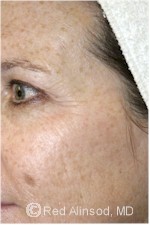 After |
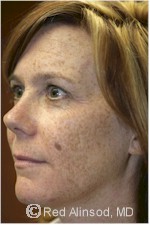 Before |
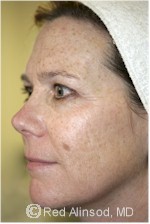 After |
Although freckles themselves are harmless, it is important to distinguish between freckles and a type of skin cancer called melanoma. If you have freckles, you have a higher risk of melanoma. Also, if your freckles are growing or changing, it is important see your physician for a skin check.
Age spots increase with age and with increased sun exposure. They are more common in people who freckle and who burn easily. It is important to know that if you’ve had enough sun to develop age spots, you have a higher risk of developing skin cancer.
Age spots are also known as sun spots, liver spots, lentigos, or lentigines. These lesions are flat, tan, brown, or dark brown spots on sun-exposed skin. As people age, sun spots most commonly appear on the backs of the hands, the forearms, neck, chest, and face. Sun spots are associated with cumulative sun exposure. The pigment producing cells in the skin (called melanocytes) are activated to produce more pigment (melanin) by ultraviolet rays. While these spots are not themselves cancerous, you may be at risk for skin cancer if you have them.
Age spots are flat and vary in size from a small pea to a dime. They usually are somewhat round and have irregular borders. They are found on chronically sun-exposed areas such as the shoulders, upper back, face, forearms, and the back of hands.
Actinic Keratosis (A Precancerous Condition)
Sun damage to the skin accumulates over time, so that even a brief exposure adds to the lifetime total.
Actinic keratosis can be the first step in the development of skin cancer, and, therefore, is considered a precancerous skin condition. The presence of actinic keratoses indicates that sun damage has occurred and that any kind of skin cancer can develop.
Actinic keratosis, also known as a solar keratosis, is a scaly or crusty bump that arises on the skin surface. The base may be light or dark, tan, pink, red, a combination of these, or the same color as the skin. The scale or crust is horny, dry, and rough, and is often recognized by touch rather than sight. Occasionally, it itches or produces a pricking or tender sensation.
It is important see a qualified physician for an annual skin check.
Treatment Options
The best treatment is prevention. The key is sun avoidance and daily sunscreen use. For example, you won’t find age spots or freckles on your inner thigh because of minimal or no sun exposure. However, for most of us, it is too late for prevention, and there are a number of treatment options available
Although it is not medically necessary to treat freckles, age spots and liver spots, patients often seek treatment for cosmetic reasons. Potential treatments include a prescription strength skin care line such as Obagi, Levulan Levulan/PhotoDynamic Therapy, chemical peels and laser or pulsed light therapy
Commonly used procedures
- Vitamin C Treatments
- Levulan/PhotoDynamic Therapy
- FotoFacial Skin Rejuvenation
- Chemical Peel
- Aesthetic Peel
- Laser Skin Resurfacing
- Palomar Fractional Skin Resurfacing
- Silk Peel
- Obagi / Blue PeelBirthmarks
Melasma
Melasma, also known as cholasma, is characterized by irregular patches of dark skin on the face and can sometimes be mistaken for a suntan that appears around the cheeks, forehead, upper lip, nose, chin, and jawline. It can also show up on the forearms, but this is quite rare. Within a patch of melasma, pigment producing cells (called melanocytes) are increased in number and each melanocyte produces more pigment (called melanin). Increased melanin in the skin leads to the tan or brown coloration.
Melasma is a common condition and is found more often in women. Those with darker skin types (including Indians, Hispanics, Middle-Easterners, and North Africans) are more prone to melasma than those with lighter complexions. Although melasma is most common in women of childbearing age, you don’t have to pregnant or even a woman to have it. It is also found in older women who did not have it during their pregnancies, and up to 10% of cases are dark skinned men.
The cause of melasma is not fully understood. However, genetics, hormonal changes, and sun exposure are known to play important roles. For example, melasma often occurs with pregnancy, hence the term “mask of pregnancy.” Oral contraceptives can also trigger melasma. Sun exposure is a big culprit. Melasma tends to darken in summer after sun exposure, and fade in winter when the sun is a rare treat. Skin inflammations from allergic reactions, or waxing of facial hair especially above the lip, can also be a trigger. Some medications can also cause melasma such as the antibiotics tetracycline and minocycline, and some anti-seizure and anti-malarial drugs.
Although there are some diseases that cause similar changes in the skin, melasma itself has no association with internal disease.
As a rule, any persistent, unexplained darkening or lightening of the skin should be looked at by a Dermatologist. The first step is to determine the cause. A complete medical history and a proper physical examination including evaluating the skin under a Wood’s lamp may be performed. Diagnostic tests, including thyroid function tests and skin biopsies, may also be done. The next step is to eliminate the cause, if possible. For example, if the cause is the medication you are taking, discontinuing it may result in a clearing, but melasma is not always that simple. The pigment may be located in the epidermis or the skin’s outer layer, the dermis or the deeper layer, or a combination of both. The more superficial it is, the easier it will lighten. In general, melasma that is more recent will respond better to treatment.
Melasma doesn’t really have a cure. In many cases associated with pregnancy, the discoloration fades away after delivery but it may persist for longer or indefinitely. The good news is that there are treatments that can be done that can minimize the visible effects and keep them at bay. There are a number of treatments available for melasma. They include: topical bleaching creams (Obagi and PCA ), sunscreens (products), chemical peels, and laser therapy.
Commonly used procedures:
- PCA
- Obagi / Blue Peel
- FotoFacial Skin Rejuvenation
- Fractional Skin ResurfacingRosacea
Handpieces that perform Pigmented Lesion Treatment:>> Fractional 1540 Erbium Laser
>> Fractional 2940 Erbium Laser
>> LuxG™
>> LuxY™
>> LuxYS™
>>Collagenizer Treatments with Vitamin C